
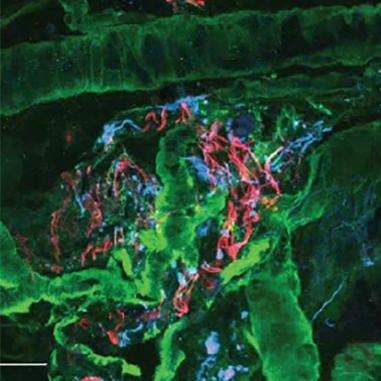
The Angio-Fibrotic Switch and Protein Networks in Proliferative Diabetic Retinopathy
Proliferative diabetic retinopathy (PDR) is a serious complication of diabetes that affects the blood vessels in the retina, the light-sensitive tissue at the back of the eye. It occurs when high blood sugar levels damage the blood vessels in the retina, causing them to leak fluid or blood. This can lead to the growth of new, abnormal blood vessels in the retina, a condition known as neovascularization. The formation of these new blood vessels is often accompanied by the formation of fibrovascular membranes, which are abnormal structures formed from scar tissue and new blood vessels that grow over the surface of the retina. Retinal traction, a condition in which the scar tissue and new blood vessels pull on the retina, causing it to become distorted or detached from its normal position, may also occur. These complications can lead to vision loss or blindness if left untreated. It is estimated that around 93 million people worldwide have diabetic retinopathy, including PDR. Early detection and treatment can help to prevent or slow the progression of PDR and reduce the risk of vision loss. Pars plana vitrectomy is an established and successful treatment for the complications of PDR. It is required in approximately 10% of patients presenting with PDR.
Publications:
Excessive VEGF production plays a critical role in the etiology of PDR and increases vascular permeability, dilates blood vessels, promotes the proliferation and migration of vascular endothelial cells, and attracts endothelial cell precursors and monocytes. Pre-operative VEGF levels have been shown to correlate with post-operative complications after vitrectomy for PDR and recently, numerous studies have reported improved clinical outcomes by injecting intravitreal bevacizumab (BVZ), ranibizumab (RZB) or aflibercept (AFB) pre-operatively in patients undergoing vitrectomy surgery for the complications of PDR. Effectivity of these drugs is related to their ability to reduce neovascular tissue vascularity, by reducing intraoperative bleeding, easing dissection of fibrovascular tissues, and by reducing the occurrence of post-operative vitreous hemorrhage.
However, next to non-responsiveness to anti-VEGF therapies in some patients, the use of anti-VEGF therapy may increase the risk of fibrotic complications, termed by us in the past as the ‘angiofibrotic switch’. We discovered a correlation between vitreous levels of the pro-fibrotic factor connective tissue growth factor (CTGF) and the degree of fibrosis in PDR patients, and demonstrated that the CTGF/VEGF ratio in vitreous was the strongest predictor of clinical fibrosis (Kuiper et al., 2008; Van Geest et al., 2012). Clinically, the angiofibrotic switch was observed after intravitreal BZB (Van Geest et al., 2013), as predicted by our experimental observations. Others have also reported exacerbation of scarring and subsequent contraction of fibrous tissue leading to tractional retinal detachment in patients who received anti-VEGF treatment for active PDR (Reviewed by Osaadon et al., 2014). Recently, applying a proteomic approach, we have identified additional proteins to CTGF that may be instrumental in the formation of fibrovascular membranes in PDR patients.
In a recent study, we conducted a large-scale screening of proteins in the vitreous and found other proteins besides CTGF that may play a role in the formation of fibrovascular membranes in PDR patients. One of these proteins is PDGF, which is capable of initiating neurite outgrowth in cultured retinas. These neurites provide a scaffold for retinal membrane formation. In a new study, we examined the role of multiple proteins in more detail in PDR patients and found that they are elevated as a group in the vitreous of these patients. We also looked at the reduction in the concentrations of these proteins after various anti-VEGF therapies.
Invest Ophthalmol Vis Sci. 2025 Jun 2;66(6):2.
Central subfield thickness of diabetic macular edema: Correlation with the aqueous humor proteome.
Mol Vis. 2024 Feb 10;30:17-35.
Vitreous protein networks around ANG2 and VEGF in proliferative diabetic retinopathy and the differential effects of aflibercept versus bevacizumab pre-treatment.
Sci Rep (2022) 12:21062.
PDGF as an Important Initiator for Neurite Outgrowth Associated with Fibrovascular Membranes in Proliferative Diabetic Retinopathy.
Curr Eye Res (2022) 47:277-286.
miRNA Levels as a Biomarker for Anti-VEGF Response in Patients with Diabetic Macular Edema.
J Pers Med (2021) 11:1297.
microRNA Expression Profile in the Vitreous of Proliferative Diabetic Retinopathy Patients and Differences from Patients Treated with Anti-VEGF Therapy.
Trans Vis Sci Tech (2020) 9:16
Identification of proteins associated with clinical and pathological features of proliferative diabetic retinopathy in vitreous and fibrovascular membranes.
PLoS One. 2017 Nov 2;12(11):e0187304.
Involvement of the ubiquitin-proteasome system in the expression of extracellular matrix genes in retinal pigment epithelial cells.
Biochem Biophys Rep. 2018 Jan 28;13:83-92.
Modulation of the Proteasome Pathway by Nano-Curcumin and Curcumin in Retinal Pigment Epithelial Cells.
Ophthalmic
Res. 2017 Oct 27.
The role of CTGF in diabetic retinopathy. Review.
Exp Eye Res. 2015;133:37-48.
Connective tissue growth factor is involved in structural retinal vascular changes in long-term experimental diabetes.
J Histochem Cytochem. 2014;62:109-18.
Vitreous TIMP-1 levels associate with
neovascularization and TGF-β2 levels but not with fibrosis in the clinical course of proliferative diabetic retinopathy.
J Cell Commun Signal. 2013 Mar;7(1):1-9.
A shift in the balance of vascular endothelial growth factor and connective tissue growth factor by bevacizumab causes the angiofibrotic switch in proliferative diabetic retinopathy.
Br J Ophthalmol. 2012 Apr;96(4):587-90.
The angio-fibrotic
switch of VEGF and CTGF in proliferative diabetic retinopathy.
PLoS One. 2008 Jul 16;3(7):e2675.
